Jho Institute for Minimally Invasive Neurosurgery Department of Neuroendoscopy
Spine Diseases
Brain Diseases
Meningioma Surgery: Dr. Jho's Endoscopic Endonasal Meningioma surgery or Mini-craniotomy Transcranial Operation
Dr. Jho's Minimally Invasive Endoscopic Endonasal surgery or Minimally Invasive Transcranial Surgery
Professor & Chair, Department of Neuroendoscopy
Jho Institute for Minimally Invasive Neurosurgery
Historically, removal of skull base meningiomas has been technically difficult with high complications. Recently, the surgical strategy of brain protection by radical extensive skull base surgery has made a significant contribution in complex skull base meningioma surgery. However, this conventional skull base surgery has been too extensive, radical and complex for patients to make easy recovery. With the combined concepts of brain protective skull base surgery and minimalism, Dr. Jho has developed minimally invasive skull base surgery. He performs meningioma tumor removal in a minimally invasive manner with the maximal protection of the brain or spinal cord.
In order to avoid complications and injury to the brain, Dr. Jho performs surgery with innovative minimally invasive techniques for complicated skull base meningiomas. Meningiomas are benign brain tumors arising from the meninges, which is the covering sheath of the brain. Meningiomas can develop in the spinal canal or in the cranial brain cavity. Although most meningiomas are benign, they can become malignant in rare occasions. Meningiomas have also been known to naturally recur even after successful total resection.
The following are examples of how Dr. Jho performs removal of meningiomas:
1. Endoscopic endonasal removal of the anterior skull base meningiomas via a nostril (without a skin incision)
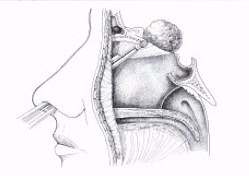
Figure 1. This schematic drawing demonstrates how anterior skull base meningiomas are removed via a nostril without any skin incisions. A 4-mm endoscope is inserted towards the base of the tumor at the skull base through a nostril. Surgical instruments are inserted next to the endoscope through the same nostril. Tumor is removed and the skull base is reconstructed. Patient's hospital stay is usually overnight.
A:  B:
B: 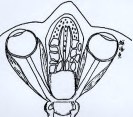
 B:
B: 
Figure 2. These schematic drawings demonstrate the area of surgical access gained by this endoscopic endonasal approach via a nostril to the anterior cranial fossa.
A: 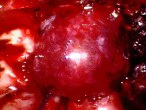 B:
B: 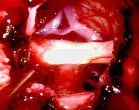
 B:
B: 
Figure 3. Intraoperative photographs show delivery of the tumor (A), the optic chiasm, pituitary stalk and anterior cerebral arteries after complete tumor removal (B).
2. Minimally invasive transcranial skull base meningioma surgery
A. Glabellar approach for anterior skull base meningiomas
A: 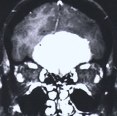 B:
B: 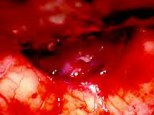 C:
C: 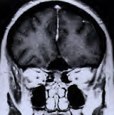
 B:
B:  C:
C: 
Figure 1. A preoperative MR scan, coronal view (A), reveals a large meningioma. An intraoperative picture (B) shows the optic chiasm and bilateral optic nerves after complete tumor removal. Postoperative MR scan (C) confirms total tumor removal through a small skin incision at the nose-bridge.
A: 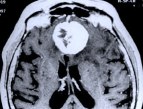 B:
B: 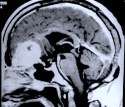 C:
C: 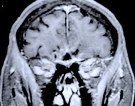 D:
D: 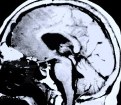
 B:
B:  C:
C:  D:
D: 
Figure 2. Preoperative MR scans, axial (A) and sagittal (B) view, disclose a large anterior fossa meningioma in an elderly woman. The tumor was totally removed under an endoscope via a 4-cm skin incision at the nose bridge. Postoperative MR scans, coronal (C) and sagittal (D) view, confirm complete removal of the tumor via a glabellar approach. A postoperative MR scan, sagittal view (D), shows an abdominal fat graft (white) placed in the ethmoid and frontal sinus in order to prevent the possibility of postoperative cerebrospinal fluid leakage.
A: 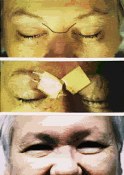 B:
B: 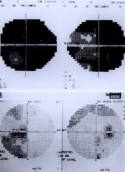
 B:
B: 
Figure 3. Pictures (A) demonstrate the line for the skin incision (Top), postoperative bandage (Middle), and the healed incision (Bottom). Preoperative visual field testing results (B: Top) display significant visual field defects portrayed by blackened areas (almost blind bilaterally). After total removal of an anterior skull base meningioma via a glabellar approach, postoperative visual field results (B: Bottom) on the same patient display significant improvement in visual fields.
A: 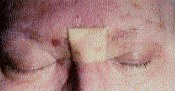 B:
B:  C:
C: 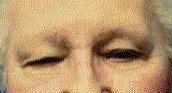
 B:
B:  C:
C: 
Figure 4. Evolution of a glabellar skin incision. When an endoscope is utilized instead of the operating microscope a much smaller incision can be used. The photograph shows a postoperative bandage placed over a skin incision (A). The skin incision at the nose bridge as seen morning after surgery (B). Healed glabellar skin incision seen six weeks following surgery (C).
B. Orbitofrontal approach via a small eyebrow incision for anterior skull base meningiomas
A: 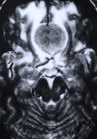 B:
B: 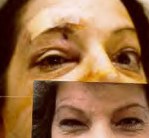 C:
C: 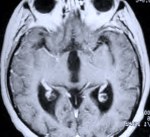 D:
D: 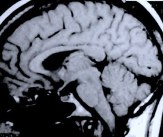
 B:
B:  C:
C:  D:
D: 
Figure 1. Preoperative MR scan, axial view (A), shows a meningioma with severe surrounding brain edema (white). Two photographs (B) of a postoperative patient show a covered eyebrow incision in the recovery room and a healed incision at 6 weeks after surgery. Postoperative MR scans, sagittal (C) and axial (D) views, confirm complete tumor removal.
A: 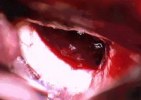 B:
B: 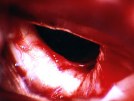
 B:
B: 
Figure 2. An intraoperative photograph (A) provides a clear image of the bilateral optic nerves and chiasm with tumor (red) adhered in a patient with a sellar meningioma. Another intraoperative photograph (B) shows the optic nerve system after complete removal of the tumor via an eyebrow incision craniotomy.
C. Subtemporal approach via a small incision for middle fossa meningiomas
A: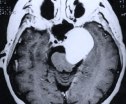 B:
B: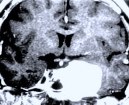 C:
C: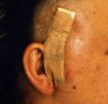 D:
D: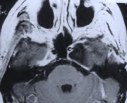 E:
E: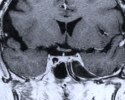
 B:
B: C:
C: D:
D: E:
E:
Figure 1. Preoperative MR scans, axial (A) and coronal views (B), reveal a large meningioma involving the cavernous sinus and tentorium. A patient wears a postoperative bandage after total tumor removal via a subtemporal approach (C). The patient did well following surgery and only experienced some residual left-sided facial numbness. Postoperative MR scans, axial (D) and coronal (E) views, confirm complete tumor removal.
D. Retromastoid approach for meningiomas at the cerebellopontine angle
When a meningioma is located at the cerebellopontine angle or lateral posterior cranial fossa, a retromastoid approach is utilized similar to an approach to an acoustic neuroma.
E. Posterolateral approach for meningiomas at the craniocervical junction
A: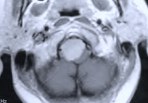 B:
B: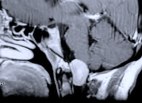 C:
C: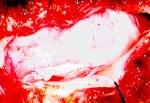 D:
D: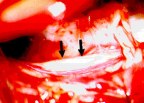
 B:
B: C:
C: D:
D:
E: 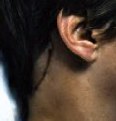 F:
F: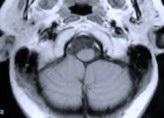 G:
G: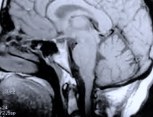
 F:
F: G:
G:
Figure 1. Preoperative MR scans, axial (A) and sagittal (B) views, reveal a meningioma that is severely compressing the medulla at the craniocervical junction. Intraoperative photographs demonstrate a large meningioma (C) and show a frontal view of the cervicomedullary junction after complete tumor removal (D). A postoperative patient photograph (E) shows the small skin incision utilized in this posterolateral approach to the craniocervical junction. Postoperative MR scans, axial (F) and sagittal (G) views, confirm complete removal of the tumor.
Practice Manager: Robin A. Coret
Tel : (412) 359-6110
Fax : (412) 359-8339
Address : JHO Institute for Minimally Invasive Neurosurgery
Department of Neuroendoscopy
Sixth Floor, South Tower
Allegheny General Hospital
320 East North Avenue
Pittsburgh, PA 15212-4772
Copyright 2002-2032


